Dr Victor Dieriks examines concerns that the rapid onset of Parkinson’s disease motor symptoms after Covid-19 infection suggests a causal link.
Since the start of this pandemic, neuroscientists have become increasingly concerned that Covid-19 could result in a surge of patients developing Parkinson’s disease.
New findings show that the problem is more acute. Three recently published case reports describe Covid-19 patients that developed clinical Parkinsonism within weeks of contracting the disease. Brain imaging revealed reduced brain function, with traditional dopaminergic medication – typically used to treat motor symptoms in Parkinson’s disease – successfully alleviating the effects for two of the three patients.
These three patients that developed clinical Parkinsonism are unique as they experienced a rapid onset of severe motor symptoms after infection by SARS-CoV-2 (the virus causing Covid-19). It is possible that they would have developed Parkinson’s disease regardless and that the viral infection only accelerated the disease progression. Nevertheless, the rapid onset of motor symptoms after SARS-CoV-2 infection suggests a causal link, mainly because none of the reported patients exhibited signs of Parkinson’s disease before their Covid-19 diagnosis or carried any known genetic risk factors.
Even though it has been more than 200 years since James Parkinson described patients with characteristic motor symptoms, we still do not know the underlying cause of Parkinson’s disease. A diagnosis is usually made when typical movement symptoms occur. It is hard to identify the disease’s exact cause as there can be as much as 50 years between the original incident and diagnosis. We know the interaction between each individual’s genetic information and the environment plays an important role, but direct links are hard to pinpoint. Epidemiological studies associate exposure to pesticides or heavy metals, traumatic brain injury, and viral/bacterial infection with an increased likelihood of developing Parkinson’s disease later in life.
Nearly every Spanish Influenza patient who had an acute episode of encephalitis (brain swelling and damage during infection) from the influenza virus went on to develop viral Parkinsonism.Covid-19 is best known as a respiratory condition, but it is evident the central nervous system is affected in a proportion of patients. The most common neurological effects observed in Covid-19 patients range from headaches, dizziness, and confusion to strokes, prolonged seizure, loss of smell, and encephalitis. The latter can escalate to a severe form known as acute disseminated encephalomyelitis, in which both the brain and spinal cord become inflamed, and neurons lose their outer coating, leading to symptoms resembling those of multiple sclerosis.
The long-term effects of Covid-19 in relation to Parkinson’s disease are still unclear, but our current knowledge does indicate several points of overlap between the disorders. In Parkinson’s disease, toxic clumps of a protein called alpha-synuclein accumulate in the brain. These alpha-synuclein clumps are first found in areas directly exposed to the outside environment — specifically, the olfactory bulbs and the gut before they appear within the brain.
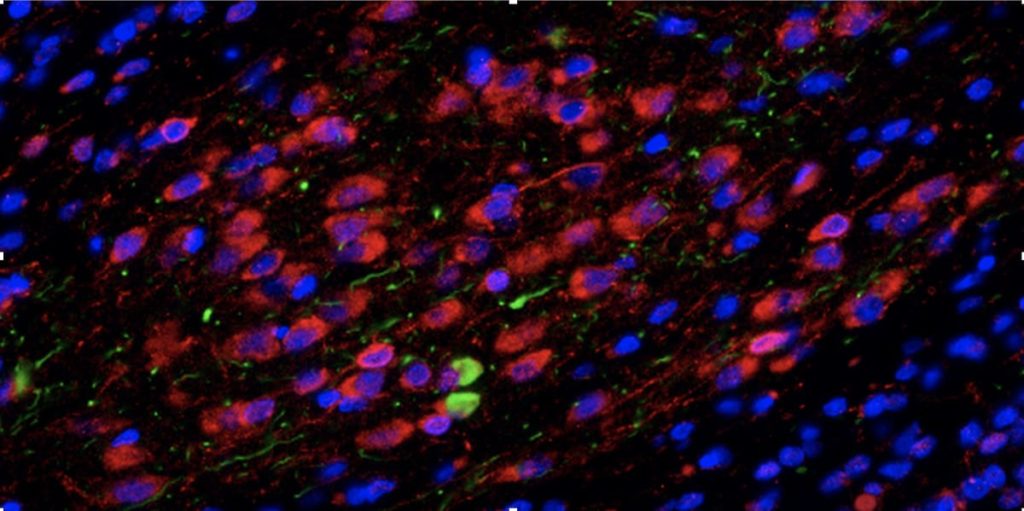
 Alpha-synuclein clumps (green) in the olfactory bulb of a Parkinson’s disease brain.
Alpha-synuclein clumps (green) in the olfactory bulb of a Parkinson’s disease brain.
Hyposmia (reduced sense of smell) and constipation are frequent features in the early disease stage of Parkinson’s disease and Covid-19, suggesting that viruses may gain direct entry to brain regions affected by Parkinson’s disease using the same routes. The SARS-CoV-2 virus infects both the upper and lower respiratory tract. This area is innervated (supplied with nerves) by the vagus nerve, which connects the brain to the lungs, providing another access point to the brain.
Researchers have long speculated that viruses do more harm than what is observed during the acute infection stage. Several findings point to a direct link with Parkinson’s disease. The most striking is the 1918 Spanish flu pandemic killing millions worldwide; those who survived were left with ongoing health issues. Nearly every Spanish Influenza patient who had an acute episode of encephalitis (brain swelling and damage during infection) from the influenza virus went on to develop viral Parkinsonism.
Epidemiologists later calculated that Spanish Influenza survivors have a two to three times higher risk of developing Parkinson’s disease compared to those who did not come into contact with the virus. Since then, viruses like the herpes simplex virus (causing cold sores in the mouth or genitalia), West Nile Virus, Western Equine Virus, and Influenza A, which causes the common flu, have all been linked to viral Parkinsonism development later in life.
Infection with these viruses can cause alpha-synuclein levels to increase – and in some cases, prompt – the formation of alpha-synuclein clumps. It is possible that SARS-CoV-2 also leads to increased alpha-synuclein levels, prompting the formation of these clumps, which could then lead to neuronal cell death. If this hypothesis is correct, SARS-CoV-2 could predispose ‘recovered’ Covid-19 patients to develop Parkinson’s disease later in life. As such, it will not be restricted to the three acute cases but could add millions to the tally and further increase the burden of our already stretched health system.
– Dr Dieriks is part of Brain Research New Zealand and Centre for Brain Research and focuses on the early effects of Parkinson’s disease. He was recently awarded a Health Research Council Sir Charles Hercus fellowship.
This article was originally published on Newsroom.



